When a patient safety issue arises, our first instinct is often to figure out who made the mistake. But this approach misses the bigger picture. Root cause analysis in healthcare is a powerful investigative process that pushes us to look beyond individual actions and uncover the systemic flaws that allowed the error to happen in the first place. It’s about fixing the system, not just pointing a finger.
Why We Must Look Deeper Than Surface-Level Errors

Patient safety problems are rarely simple, isolated events. Treating them that way is like putting a bucket under a leaky ceiling—sure, you've contained the immediate mess, but you haven't fixed the burst pipe hidden in the wall. You can be certain the problem will show up again. This is exactly where root cause analysis (RCA) offers a much more durable solution.
Think of an RCA investigator as a detective. Instead of just identifying a suspect and closing the case, they meticulously reconstruct the entire chain of events. They ask why the security system failed, why the lock was broken, and why the alarm never went off. This deeper line of questioning reveals hidden weak spots in processes, communication breakdowns, or environmental factors that set the stage for the incident.
The Wake-Up Call for Patient Safety
The critical need for this kind of systematic approach was cemented by a landmark 1999 report from the Institute of Medicine (IOM). The report revealed a staggering reality: more patients were dying from preventable medical errors each year than from car accidents or breast cancer. The estimates were shocking, suggesting up to 400,000 hospitalized patients suffered preventable harm annually, with costs soaring into the billions.
That report was a true turning point, establishing RCA as an essential process for creating safer healthcare environments. You can explore these findings in more detail on the NCBI Bookshelf.
A culture of safety is not a culture of blame. It is a culture that enables people to learn from their mistakes and to feel comfortable reporting them.
This distinction is absolutely vital. Blaming an individual is like treating a symptom while ignoring the underlying disease. For example, if a patient is given the wrong medication, the easy answer is to blame the nurse who administered it. A proper RCA, however, might uncover that the real root cause was a poorly designed electronic health record (EHR) interface that made it far too easy to select the wrong drug.
Fostering a Culture of Continuous Learning
By shifting the focus from individual fault to systemic flaws, RCA helps build a genuine culture of safety. It creates an environment where staff feel secure enough to report near-misses without fearing punishment.
This kind of transparency is the fuel for continuous improvement and is vital for any practice, including chiropractic care. Just as we look for the underlying reasons for a patient's physical symptoms, understanding the root causes of our clinical and operational challenges is essential for growth. You can see this approach in action by reading our guide on understanding the root causes of ADHD in children.
What Is Root Cause Analysis, Really?
Let’s get past the jargon. At its heart, root cause analysis in healthcare is just a structured way of asking “Why?” until you get to the real source of a problem. It’s not about patching things up for the day; it’s about making changes so the issue never comes back. Think of it as a methodical process for digging past the obvious “what happened” to uncover the foundational “why it happened.”
Imagine you walk into your clinic and find a puddle of water on the floor. The immediate reaction is to grab a mop and clean it up. That takes care of the symptom—the water—but it does nothing to stop another puddle from showing up tomorrow.
A root cause analysis approach is like calling a plumber. They don't just mop; they trace the water back through the walls until they find the leaky pipe. Fixing that pipe is the only way to solve the problem for good. That’s the critical difference between reacting to problems and truly resolving them.
Symptoms vs. Root Causes
In a busy practice, it’s all too easy to get stuck putting out fires. These immediate problems are usually just symptoms of something deeper going on. We call these surface-level triggers contributing factors. They’re the obvious, immediate reason something went wrong. The root cause, however, is the hidden weakness in your system that allowed it to happen in the first place.
Here’s a simple way to see the difference:
- Contributing Factor: A patient misses their appointment because they wrote down the wrong time. This is the immediate cause.
- Root Cause: Your clinic's automated reminder texts are worded in a confusing way, causing patients to frequently mix up their appointment times. This is the systemic flaw.
Calling the patient to reschedule fixes the problem for that one person, that one time. Rewriting the automated text message fixes the root cause and prevents dozens of future missed appointments.
Root cause analysis shifts the focus from asking, "Who made a mistake?" to "What part of our system let this mistake happen?" This one change in perspective is the key to building a safer, more reliable practice.
Why This Distinction Is So Important
One of the biggest pitfalls in any clinic is not digging deep enough. When we only treat symptoms or contributing factors, we get trapped in a frustrating cycle of fixing the same problems over and over. It drains energy, creates inefficiencies, and can even put patient safety at risk. In fact, The Joint Commission has found that a huge number of serious safety events can be traced back to systemic issues that were never properly addressed.
A true root cause analysis pushes your team to keep asking probing questions until there are no more questions to ask. It forces you to hit pause and look at the processes, communication, and tools you rely on every day. That deeper understanding is what turns a one-off incident into a powerful opportunity for real, lasting improvement.
Proven RCA Methods for Your Healthcare Team
Once you understand why digging for the root cause is so crucial, the next step is learning how to use the right tools for the job. Just like a chiropractor chooses a specific technique for an adjustment, your healthcare team needs to select the right investigative method for the problem at hand. These proven methods give you a structured framework to guide your team from the initial incident all the way to a meaningful, lasting solution.
The goal isn't just to have another meeting; it's to run a focused, productive investigation. Moving beyond unstructured brainstorming is the key to uncovering genuine systemic flaws instead of just pointing fingers at surface-level issues. Each method offers a unique lens to view a problem, ensuring no stone is left unturned.
The 5 Whys A Simple Path to Deeper Insight
Maybe the most straightforward—and surprisingly powerful—tool in the RCA toolbox is the 5 Whys method. It’s built on a simple but profound idea: by repeatedly asking "Why?" you can peel back the layers of a problem to get to what’s really going on. Think of it as channeling a child's relentless curiosity into a potent diagnostic tool.
Imagine a medication error happens in your clinic—a patient gets the wrong dosage. A surface-level investigation might stop after the very first "why."
- Problem: A patient received the wrong medication dose.
- Why? The nurse administered the incorrect amount from the vial. (This is just the surface.)
- Why? The vial pulled from the automated dispensing cabinet was the wrong concentration.
- Why? The pharmacy technician had stocked the cabinet with the incorrect vial.
- Why? Two medications with very similar packaging and names were stored right next to each other in the pharmacy.
- Why? The clinic’s inventory management protocol doesn't require separating look-alike, sound-alike drugs. (Now we're at the root cause.)
See how the focus shifts? It moves from an individual action (the nurse's mistake) to a systemic flaw (a faulty inventory protocol). The real solution isn't just telling people to "be more careful"; it’s a concrete action like reorganizing pharmacy storage to make sure this kind of error can't happen again.
The Fishbone Diagram Visualizing Complex Problems
For more complex issues that have multiple potential contributing factors, the Fishbone Diagram is invaluable. It's also known as an Ishikawa or Cause-and-Effect Diagram. This visual tool helps teams brainstorm and organize all the potential causes into distinct categories, creating a comprehensive map of the problem.
Think of the "head" of the fish as the problem you're trying to solve (e.g., "Increase in Patient Falls on the West Wing"). The "bones" branching off the spine represent different categories of potential causes.
A Fishbone Diagram is fantastic for preventing "groupthink." It encourages the team to explore multiple cause categories instead of getting fixated on the most obvious one, forcing a much broader and more systematic perspective.
In a healthcare setting, your categories might include things like:
- People: Staffing levels, training gaps, communication breakdowns, fatigue.
- Processes: Admission protocols, patient handover procedures, medication administration workflow.
- Equipment: Malfunctioning bed alarms, broken call bells, poor lighting.
- Environment: Room clutter, high noise levels, time of day.
- Materials: Lack of non-slip socks, unavailable assistive walking devices.
By mapping out all the possibilities, your team can visually identify where the most significant weaknesses are. This guides a more targeted and effective investigation, ensuring your final root cause analysis in healthcare is thorough and considers every angle.
This infographic shows how these two popular RCA methods are used in practice and their impact on efficiency.
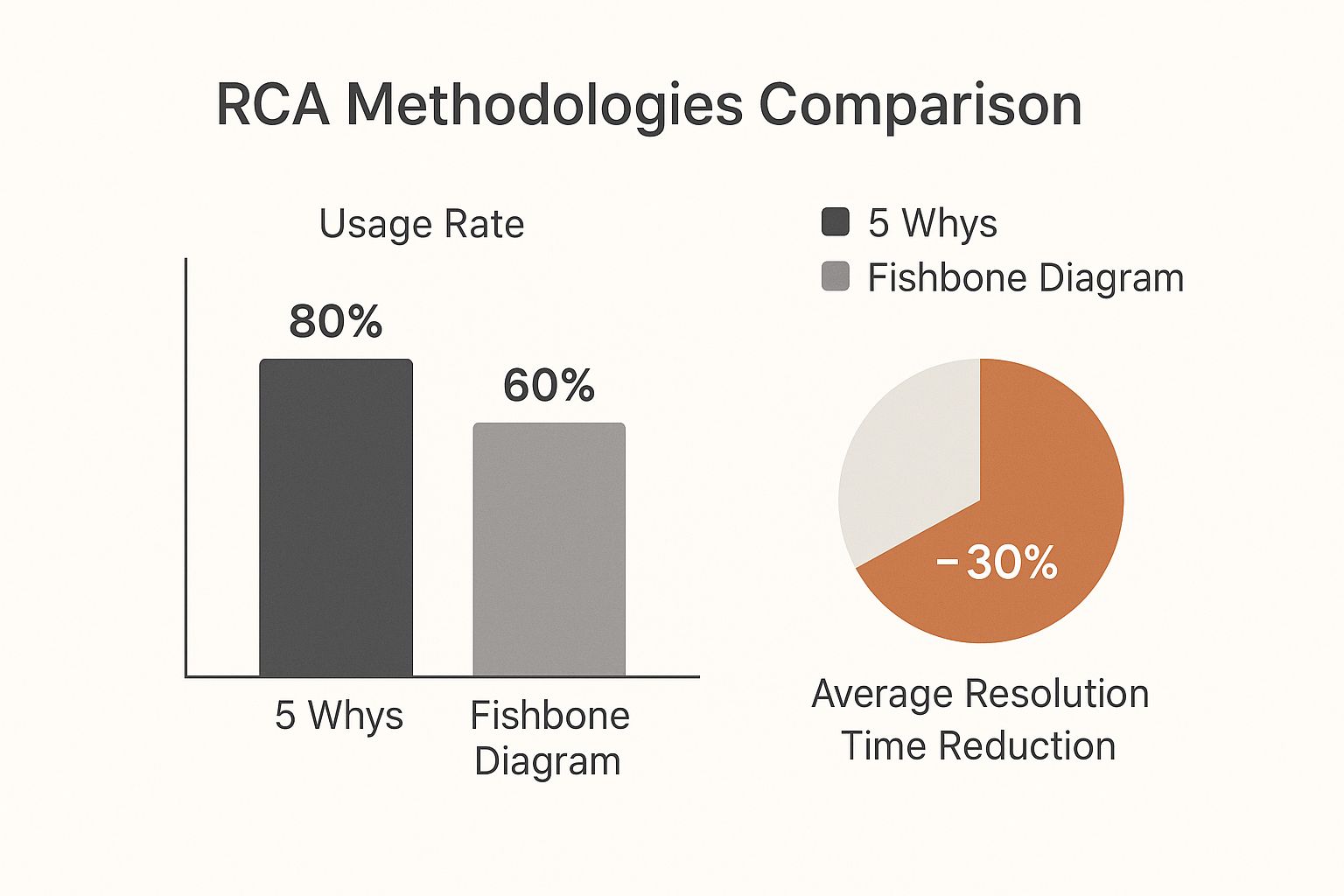
The data shows that while the simpler 5 Whys method is used more often, both tools lead to a significant drop in the time it takes to resolve the underlying issues for good.
Comparing Common RCA Methodologies in Healthcare
Choosing the right tool is the first step toward a successful investigation. Not every method fits every problem. This table breaks down the most common RCA tools to help you decide which one is the best fit for the situation your clinic is facing.
| Methodology | Best For | Key Feature | Complexity Level |
|---|---|---|---|
| 5 Whys | Simple to moderately complex problems with a single, linear cause. | Its simplicity. A quick, straightforward way to drill down past surface-level symptoms. | Low |
| Fishbone Diagram | Complex problems with multiple potential contributing factors across different areas. | Visual brainstorming. Helps organize many ideas into logical categories. | Moderate |
| Fault Tree Analysis (FTA) | High-risk, complex system failures, especially those involving technology or equipment. | Top-down deductive logic. Starts with the failure and works backward to find all possible causes. | High |
Each of these methods provides a structured pathway to uncover the truth. The key is matching the complexity of your tool to the complexity of the problem you're trying to solve.
Fault Tree Analysis A Top-Down Approach
Another powerful tool your team can use is Fault Tree Analysis (FTA). This method works in the opposite direction of a Fishbone Diagram. It starts with a specific failure or undesirable event (the "top event") and works backward to identify all the potential causes—both human and mechanical—that could have led to it.
For instance, the top event could be "EHR system downtime during clinic hours." The analysis would then branch down to explore all the possible contributing factors, like a software failure, a hardware malfunction, network issues, or even a simple user error.
FTA is particularly effective for analyzing technical system failures and pinpointing critical points of vulnerability. When you understand all the pathways that can lead to failure, your team can implement targeted, preventative measures to make the whole system more reliable.
How Effective RCA Transforms Your Practice

Bringing root cause analysis in healthcare into your practice isn't just about ticking a box for compliance—it's a genuine commitment to making your entire organization better. The benefits go far beyond a single investigation, creating positive ripple effects that improve patient safety, smooth out operations, and build a more resilient team.
When you consistently dig deeper to find out why mistakes happen, you finally break that frustrating cycle of the same problems popping up over and over. Instead of just slapping a bandage on a recurring issue, you develop solid, system-wide solutions that prevent it from happening again. This proactive mindset is the real foundation of excellent patient care.
Elevating Patient Safety and Quality of Care
The single biggest win from effective RCA is its direct impact on patient safety. Globally, the numbers are sobering. The World Health Organization finds that 1 in 10 patients is harmed while receiving medical care, leading to millions of preventable deaths each year. RCA is one of the most powerful tools we have to unpack these events and strengthen the very systems meant to protect our patients. You can discover more about these global patient safety challenges on who.int.
By uncovering those hidden weak spots in your clinical and administrative workflows, you can make smart, targeted improvements. This doesn't just lead to safer care; it leads to better outcomes and happier, more confident patients. A well-done RCA can show you how to optimize everything from your front desk scheduling to how patient information is handed off between staff.
Shifting from a Blame Culture to a Learning Culture
Maybe the most profound change RCA brings is a cultural one. In a traditional, reactive setting, the first response to a mistake is often to find someone to blame. This creates a toxic "blame culture" where staff become afraid to report errors or even near-misses, fearing they'll be punished.
RCA dismantles this destructive cycle by shifting the focus from individual fault to systemic flaws. It fosters a "learning culture" where errors are viewed not as failures, but as valuable opportunities to understand and improve the system.
This shift does wonders for team morale and psychological safety. When your team members feel safe enough to speak up, they become your practice's best line of defense against future errors. They’ll be more likely to flag small issues before they snowball into major incidents, creating a powerful cycle of continuous improvement.
For example, just as we work to identify the root cause of a patient's recurring headaches to create a better treatment plan, we can use the same thinking to understand a clinical error to create better safety protocols. You can learn more about how we approach finding the root causes of headaches in our detailed guide.
Realizing Tangible Financial Returns
Beyond the priceless gains in safety and culture, a commitment to root cause analysis also brings real financial benefits. When you prevent adverse events, you dramatically cut the costs that come with them.
Here’s what that looks like:
- Lowered Litigation Risks: When you proactively fix systemic issues, you reduce the chances of malpractice claims down the line.
- Reduced Operational Waste: Fixing inefficient processes saves time and resources that used to be wasted on do-overs and managing the same old problems.
- Improved Patient Retention: A reputation for safety and quality is one of the strongest drivers of patient loyalty and new referrals.
Ultimately, investing time in a thorough RCA isn't an expense—it's an investment in the long-term health and stability of your practice.
Putting RCA Into Action in a Chiropractic Setting

The principles of root cause analysis in healthcare aren't just for big, bustling hospitals with dedicated safety committees. Far from it. These investigative tools are surprisingly flexible and can bring incredible value to a focused, patient-centered practice like yours.
The real key is adopting the same curious, "why-driven" mindset and applying it to the unique challenges that pop up in your clinic every day. When you translate these methods to a chiropractic setting, you can finally shift from just reacting to problems to proactively making your systems stronger. This change improves everything—from clinical outcomes and patient communication all the way to how smoothly your front desk operates.
Let’s walk through how to put these ideas into practice with a couple of scenarios you’ve probably seen before.
Case Study Using the 5 Whys
Imagine a patient calls to report feeling unexpectedly sore the day after their adjustment—more than the typical sensation you normally discuss. It’s not a major crisis, but it's a patient satisfaction issue that deserves a closer look. Instead of just reassuring them, your team decides to dig in with the 5 Whys.
- Why did the patient feel so sore?
- Because they did two hours of strenuous yard work a few hours after their appointment.
- Why did they do yard work when it was a bad idea post-adjustment?
- They said they weren't aware of any specific activity restrictions for that day.
- Why weren't they aware?
- The chiropractor gave them verbal instructions, but the patient was distracted trying to manage two young kids at checkout and didn't really hear them.
- Why did we only rely on verbal communication at such a busy time?
- Our standard procedure has always been just verbal instruction; we don't have a consistent follow-up method to reinforce it.
- Why don't we have a follow-up method?
- We haven’t created a simple take-home instruction sheet or set up an automated text with post-adjustment guidelines. (This is the root cause.)
See what happened? The analysis shows the problem wasn't the adjustment itself, but a simple gap in the patient communication process. The fix isn't to just "talk slower" next time. It’s to implement a system-wide solution, like a standardized handout that backs up your verbal advice.
Root cause analysis turns a single patient complaint into a system-wide improvement. By addressing the communication gap, you prevent dozens of similar misunderstandings in the future, enhancing care for everyone.
Using a Fishbone Diagram for Operational Issues
Now, let's look at a different kind of headache: scheduling errors. Your front desk is consistently dealing with complaints about patients showing up on the wrong day or appointments being booked for the incorrect length of time. The easy reaction is to blame the staff, but that’s rarely the whole story. A simple Fishbone Diagram can uncover what’s really going on.
Your team could brainstorm potential causes under a few key categories:
- People: Is there a training gap with the new software update? Is the front desk understaffed during peak call times, forcing them to rush?
- Process: Is the procedure for booking a new patient versus a follow-up clear? Is there a set workflow for handling rescheduling requests?
- Technology: Is the scheduling software interface confusing or glitchy? Do the automated reminders sometimes send conflicting information?
- Environment: Is the front desk area too loud, making it hard to hear patients clearly on the phone?
This visual approach often reveals that the "obvious" cause is just one piece of a much larger puzzle. You might find the root cause isn't staff error but a confusing software update combined with the lack of a standardized booking script. Armed with that knowledge, you can provide targeted training and create clear process documents—real solutions that actually stick.
Navigating the Common Pitfalls of RCA
Running a root cause analysis sounds straightforward, but in reality, it's often far more challenging than it looks on paper. Even with the best of intentions, healthcare teams can easily stumble into common traps that weaken the entire process, leading to flimsy solutions and the same problems popping up again and again.
Knowing what these pitfalls are is the first step to avoiding them.
One of the most frequent mistakes is simply stopping the investigation too early. A team might identify an immediate cause, like a staff member who didn't follow a specific protocol, and consider the case closed. This kind of surface-level analysis completely misses the deeper, systemic issues—like why the protocol was so hard to follow in the first place.
Another major hurdle is confirmation bias. This is where the team unconsciously looks for evidence that confirms what they already think went wrong. This tunnel vision can make them completely ignore critical information pointing to a different, less obvious root cause.
Overcoming Blame and Time Constraints
The pull toward a culture of blame is a powerful force that can completely derail an RCA. When people fear being punished, they naturally become defensive. The focus shifts from fixing a broken system to protecting individuals, which makes the honest, open dialogue needed for a real analysis totally impossible.
On top of that, healthcare professionals are almost always short on time. A proper RCA isn’t something you can squeeze in between appointments; it requires dedicated, protected time for the team to gather data, meet, and really think through the issues. Without this commitment from leadership, investigations get rushed, and the conclusions are often incomplete or just plain wrong.
A systematic review from 2020 highlighted these exact challenges. While it confirmed that communication breakdowns and human errors were common root causes, it also questioned how effective RCA is in the real world. The review found that 15% of studies reported improper use of RCA methods. In some situations, a staggering 65% of investigations were conducted incompletely. You can learn more about these RCA effectiveness findings.
Strategies for a Successful RCA
To steer clear of these challenges, it’s vital to build a solid foundation for your investigation from the start. Here are a few practical strategies to keep your RCA on the right track:
- Build a Multidisciplinary Team: Your team should include people from different roles and departments. A diverse group brings a variety of perspectives to the table, which is one of the best ways to fight confirmation bias and see the full picture.
- Secure Protected Time: Leadership has to formally set aside time for the RCA. This sends a clear message that the process is a priority and gives the team the breathing room they need to do a thorough job.
- Focus on System-Level Solutions: The ultimate goal should always be to create strong fixes at the system level. Instead of just recommending "more training" (which is often a weak fix), focus on improving processes, checklists, or technology to make it much harder for errors to happen in the first place. For instance, we apply this same deep-dive thinking when navigating the challenges of tongue ties in newborns to ensure comprehensive care.
A successful root cause analysis doesn't end with finding a cause; it ends with implementing a robust solution that makes the system safer for every patient and team member.
Your Questions About Root Cause Analysis Answered
Even with a solid grasp of the methods, kicking off a formal root cause analysis can feel a little intimidating. Let's walk through some of the most common questions that pop up when healthcare teams start weaving these powerful tools into their daily work.
How Often Should We Be Doing an RCA?
A root cause analysis in healthcare is an absolute must after any major patient safety issue or adverse event. But you shouldn't just wait for a crisis to happen.
The real magic comes from using RCA proactively. Look at the near-misses or those small, recurring frustrations—like those pesky scheduling mistakes that keep happening. Tackling these little things with a quick RCA can stop a much bigger problem from ever taking root. High-performing teams make this a regular habit, not just a reaction to something going wrong.
Who Should Be on the RCA Team?
Pulling together the right team is critical, and it’s a huge mistake to only include managers or department heads. The best insights come from a multidisciplinary group of people who are actually involved in the process you're looking at.
A strong team needs voices from every level. You'll want to include:
- Frontline Staff: The nurses, technicians, or administrators who live and breathe this system every single day.
- Leadership: A manager or team lead who has the authority to approve and roll out changes.
- Subject Matter Experts: Someone who knows the specific clinical or operational area inside and out.
A diverse team is your best defense against blind spots and bias. When people from different roles look at the same problem, they bring unique perspectives that help uncover the real, often hidden, root cause.
Is RCA Just for Big Hospitals?
Not at all. The core ideas behind RCA are completely scalable. They're just as valuable for a solo chiropractic clinic as they are for a massive hospital network. You just have to adjust the tools to fit the size of the problem.
In a small practice, a quick "5 Whys" chat with two or three people can be just as effective as a formal, weeks-long investigation at a larger facility. The goal is always the same: get past the symptoms to find and fix the real issue. It’s all about adapting the process to fit your team and your resources.
At First Steps Chiropractic, we don't just apply a root-cause approach to our office processes—we bring that same thinking to our patient care. We believe in addressing foundational issues to build lasting wellness. To see our neurologically-focused approach in action, visit us online.

